TRACHEOSTOMY CARE and tracheal suctioning are high-risk procedures. To avoid poor outcomes, nurses who perform them—whether they’re seasoned veterans or novices—must adhere to evidence-based guidelines. In fact, experienced nurses may overestimate their own trach care competence. Tracheostomy patients aren’t seen only in intensive care units. As patients with more complex conditions are admitted to hospitals, an increasing number are being housed on general nursing units. Trach patients are at high risk for airway obstruction, impaired ventilation, and infection as well as other lethal complications. Skilled bedside nursing care can prevent these complications. This article describes evidence-based guidelines for tracheostomy care, focusing on open and closed suctioning and site care.
Suctioning a trach tube
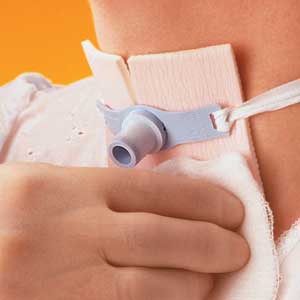 A trach tube may have a single or double lumen; it may be cuffed or uncuffed, fenestrated (allowing speech) or unfenestrated. Each variation requires specific management. For instance, before suctioning a fenestrated tube, you must insert a plain inner tube, because a suction catheter may puncture the small opening of the fenestrated tube. (See Trach tube positioning by clicking the PDF icon above.) Regardless of the type of tube used, suctioning always involves:
A trach tube may have a single or double lumen; it may be cuffed or uncuffed, fenestrated (allowing speech) or unfenestrated. Each variation requires specific management. For instance, before suctioning a fenestrated tube, you must insert a plain inner tube, because a suction catheter may puncture the small opening of the fenestrated tube. (See Trach tube positioning by clicking the PDF icon above.) Regardless of the type of tube used, suctioning always involves:
- assessment
- oxygenation management
- use of correct suction pressure
- liquefying secretions
- using the proper-size suction catheter and insertion distance
- appropriate patient positioning
- evaluation.
Also, be sure to keep emergency equipment nearby. (See Be prepared for trach emergencies by clicking the PDF icon above.)
When to suction
Suctioning is done only for patients who can’t clear their own airways. Its timing should be tailored to each patient rather than performed on a set schedule. Start with a complete assessment. Findings that suggest the need for suctioning include increased work of breathing, changes in respiratory rate, decreased oxygen saturation, copious secretions, wheezing, and the patient’s unsuccessful attempts to clear secretions. According to one researcher, fine crackles in the lung bases indicate excessive fluid in the lungs, and wheezing patients should be assessed for a history of asthma and allergies.
Suctioning technique
Before suctioning, hyperoxygenate the patient. Ask a spontaneously breathing patient to take two to three deep breaths; then administer four to six compressions with a manual ventilator bag. With a ventilator patient, activate the hyperoxygenation button. Experts recommend using suction pressure of up to 120 mm Hg for open-system suctioning and up to 160 mm Hg for closed-system suctioning. For each session, limit suctioning to a maximum of three catheter passes. During catheter extraction, suctioning can last up to 10 seconds; allow 20 to 30 seconds between passes. For open-system suctioning, catheter size shouldn’t exceed half the inner diameter of the internal trach tube. To determine the appropriate-size French catheter, divide the internal trach tube size by two and multiply this number by three. A #12 French catheter is routinely used for closed suctioning. Premeasure the distance needed for insertion. Experts suggest 0.5 to 1 cm past the distal end of the tube for an open system, and 1 to 2 cm past the distal end for a closed system.
Liquefying secretions
The best ways to liquefy secretions are to humidify secretions and hydrate the patient. Do not use normal saline solution (NSS) or normal saline bullets routinely to loosen tracheal secretions because this practice:
- may reach only limited areas
- may flush particles into the lower respiratory tract
- may lead to decreased postsuctioning oxygen saturation
- increases bacterial colonization
- damages bronchial surfactant.
Despite the potential harm caused by NSS use, one survey found that 33% of nurses and respiratory therapists still use NSS before suctioning. Other researchers have found that inhalation of nebulized fluid also is ineffective in liquefying secretions.
Evaluation
When evaluating the patient after suctioning, assess and document physiologic and psychological responses to the procedure. Convey your findings verbally during nurse-to-nurse shift report and to the interdisciplinary team during daily rounds.
Trach site care and dressing changes
Tracheostomy dressing changes promote skin integrity and help prevent infection at the stoma site and in the respiratory system. Typically, healthcare facilities have both formal and informal policies that address dressing changes, although no evidence suggests a particular schedule of dressing changes or specific supplies for secretion absorption must be used. On the other hand, the evidence does show that:
- secretions can cause maceration and excoriation at the site
- the site should be cleaned with NSS
- a skin barrier should be applied to the site after cleaning
- loose fibers increase the infection risk
- the trach tube should be secured at all times to prevent accidental dislodgment, using the two-person securing technique described below under “Securing the trach tube.”
Start by assessing the stoma for infection and skin breakdown caused by flange pressure. Then clean the stoma with a gauze square or other nonfraying material moistened with NSS. Start at the 12 o’clock position of the stoma and wipe toward the 3 o’clock position. Begin again with a new gauze square at 12 o’clock and clean toward 9 o’clock. To clean the lower half of the site, start at the 3 o’clock position and clean toward 6 o’clock; then wipe from 9 o’clock to 6 o’clock, using a clean moistened gauze square for each wipe. Continue this pattern on the surrounding skin and tube flange. Avoid using a hydrogen peroxide mixture unless the site is infected, as it can impair healing. If using it on an infected site, be sure to rinse afterward with NSS.
Dressing the site
At least once per shift, apply a new dressing to the stoma site to absorb secretions and insulate the skin. After applying a skin barrier, apply either a split-drain or a foam dressing. Change a wet dressing immediately.
Securing the trach tube
Use cotton string ties or a Velcro holder to secure the trach tube. Velcro tends to be more comfortable than ties, which may cut into the patient’s neck; also, it’s easier to apply. The literature overwhelmingly recommends a two person technique when changing the securing device to prevent tube dislodgment. In the two-person technique, one person holds the trach tube in place while the other changes the securing device.
Review trach tube policy and procedures
To achieve positive outcomes in patients with trach tubes, keep abreast of best practices and develop and maintain the necessary skills. Every nurse who performs trach care needs to be familiar with facility policy and procedure on trach tube care. If your facility’s current policy and procedures don’t support evidencebased practice, consider urging colleagues and managers to conduct a patient-care study comparing different approaches to suctioning. Then follow the evidence by advocating for changes if necessary.
Selected references
Chulay M. Suctioning: endotracheal or tracheostomy tube. In: Wiegand DJ, Carlson KK, eds. AACN Procedure Manual for Critical Care. 6th ed. Philadelphia, PA: Elsevier Saunders; 2010:62-70.
Dennis-Rouse MD, Davidson JE. An evidence-based evaluation of tracheostomy care practices. Crit Care Nurs Q. 2008;31(2):150-160.
Edgtton-Winn M, Wright K. Tracheostomy: a guide to nursing care. Aust Nurs J. 2005;13(5):1-4.
Harkreader H, Hogan MA, Thobaben M. Fundamentals of Nursing: Caring and Clinical Judgment. 3rd ed. Philadelphia, PA: Saunders; 2007.
Klockare M, Dufva A, Danielsson AM, et al. Comparison between direct humidification and nebulization of the respiratory tract at mechanical ventilation: distribution of saline solution studied by gamma camera. J Clin Nurs. 2006;15(3):301-307.
Kuriakose A. Using the Synergy Model as best practice in endotracheal tube suctioning of critically ill patients. Dimens Crit Care Nurs. 2008;27(1):10-15.
Lewis SL, Dirksen SR, Heitkemper MM, Bucher L, Camera I. Medical-Surgical Nursing: Assessment and Management of Clinical Problems. 8th ed. St. Louis, MO: Mosby; 2010.
Smith-Miller C. Graduate nurses’ comfort and knowledge level regarding tracheostomy care. J Nurses Staff Dev. 2006;22(5):222-229.
Wiegand DJ, Carlson KK, eds. AACN Procedure Manual for Critical Care. 6th ed. Philadelphia, PA: Elsevier Sauders; 2010.
Betty Nance-Floyd is a clinical assistant professor at the University of North Carolina at Chapel Hill School of Nursing.


















18 Comments.
Are LPNs performing deep suctioning? How do you define deep suctioning? Who trains the LPN?Can this be done in the home by this LPN with no RN in the home or available other than by phone?
I’m a Lary since 9/2018. I have never added moisture to my trachea (deliberately but have had a few rough showers) post op and rarely cover stoma with foam or baseplate/HME. Just bandanna or naked is most comfortable for me. Mucus production is excessive but I have a muscular build and really strong cough so I rarely fight for air.
Does anyone have home vents on their Pediatric floor? What is your nurse to patient ratio?
hey I’m researching papers comparing saline vs tap water to clean inner tubes, does anyone have any recent up to date papers or trails on it?
More help means less error.
More help means less profit.
You lose.
Just be a nurse for the money. Screw management
@Lawrencesmom: I am so disgusted to hear your story, and I am so incredibly sorry to hear what your son and family endured due to complete disregard for human life. Whoever that nurse was, you need to get their name and you need to turn her in to the State. I will give you the information myself on how to do this if you need it(OR-google) Your son DESERVES that after what he endured at his/her handsThis nurse will kill patients if allowed to continue to practice,if they havent already…GodBless
Does anyone know of a nursing home that accept patient with a trach in the Atlanta GA area?
Lawrencesmom- That`s a disgrace to the nursing profession. Those people are accountable to a nurses board and you can probably take it there if you are getting nowhere with the institution. I am very sorry that your son has not had the professional care he deserves. All staff have a duty of care. Take it to the administration.You have enough to worry about.
if normal saline solution is not allowed, what is the appropriate solution to use for suctioning?
regarding tracheostomy sutures:this is our practice can remove flange holding suture after 7days (trach will be formed)and all other sutures after 2 weeks…Regarding stoma dressing we use plymem (shapes)tube dressing for infected case and precut soft gause for non infected cases and uses vaselin also..
My son at age 18 had a tracheostomy due to illness. later was sent to a Rehab. facility for decanulation. Born with Down Syndrome,prior heart surgeries,sleep apena,COPD, he was,or should have been considered high risk.My son was completely disregarded, not monitored properly,hydration and fluids were not maintained.He suffered severe dehydration and suffocation,cross contamination etc.Answers to proper care needed.Respiratory therapist was dumping contaminated fluids in tubing back dwn into lung
does anyone know of a nusing home that will take patients with a trach
An “ok” article with two exceptions. #1: it says to listen to the lung bases for effectiveness of suctioning – NO!, listen over the carina and main stem bronchi, the actual areas where suctioning takes place. #2, it doesn’t emphasize the importance of keeping the bottom of the trach plate off the skin to prevent a decubitus ulcer.
Additionally, the article discusses placement of the dressing but does not deal with the problem of having sutures in the way – a common problem.
Trach site skin barrier: Currently, there is no specific skin barrier used for trach sites. Follow your hospital or facility policy. Many hospitals use a generic moisture barrier that can also be used for sensitive skin to prevent skin breakdown. If the surrounding tissue is intact, you could use a protective barrier wipe. The wipe in non-irritating and provides a topical barrier between the skin and tape or an appliance. Caution: The wipe contains alcohol and should not be used on open sk
The normal humidification system is bypassed with trach patients. Humidification must be supplemented. A t-tube to administer humidified oxygen can be used to liquefy the secretions. This technique is generally used in the hospital setting. At home, many patients use distilled water and saline reservoirs in a humidification system. Reservoirs should be used with caution as they can be a source of infection unless cleaned properly.
Betty Nance-Floyd
When suctioning a closed or an open system, sterile technique should certainly be used. Cleaning the trach site and dressing change is a clean procedure. At this point, no literature supports clean technique for trach suctioning.
Betty Nance-Floyd
How about emphasizing the use of sterile technique as well? Is there any literature that supports clean over sterile, if not, sterile should be used.
Under liquefying secretions, how do you recommend humidifying secretions? Article stated what NOT to do, but not what TO do.
Trach site care. What is the recommended skin barrier?