Follow these steps to ensure nurse engagement and interprofessional collaboration.
Takeaways:
- Creating a PPM is required for ANCC Magnet® designated facilities.
- Establishing and modifying the PPM requires engagement by clinical nurses and nurse leaders to reflect nursing culture and professional values.
- The PPM must align with the organizational strategic vision; organizational changes may require adaption of the PPM so it remains current.
By Wendy Silverstein, DNP, RN-BC, CNML, CPHQ, and Mildred Ortu Kowalski, PhD, RN, NE-BC, CCRP
Developing a professional practice model (PPM) can be challenging. Some within
an organization may not understand what a PPM is, the role it plays, or the impact it has on professional practice.
 The American Nurses Association (ANA) underscores the importance of a PPM for each American Nurse Credentialing Center Magnet®-recognized organization. (See Professional practice model defined.) PPMs have been linked to quality care, nurse satisfaction, and nurse engagement. In addition, they reflect the values of nursing staff and help direct care.
The American Nurses Association (ANA) underscores the importance of a PPM for each American Nurse Credentialing Center Magnet®-recognized organization. (See Professional practice model defined.) PPMs have been linked to quality care, nurse satisfaction, and nurse engagement. In addition, they reflect the values of nursing staff and help direct care.
The commitment to a PPM includes keeping it current to adapt to changes within health care. An annual evaluation of the PPM ensures that it remains an accurate reflection of the focus and efforts within the organization.
This article provides a blueprint for nurses who plan to create or adapt a PPM.
Professional practice model definedThe American Nurses Credentialing Center Magnet Application Manual defines a professional practice model as “the overarching conceptual framework for nurses, nursing care, and interprofessional patient care. It is a schematic description of a system, theory, or phenomenon that depicts how nurses practice, collaborate, communicate, and develop professionally to provide the highest-quality care for those served by the organization (e.g., patients, families, communities).” |
PPM process steps
We followed several well-defined steps in the creation of our PPM. We conducted a literature review, defined key attributes of the PPM, ensured nurse engagement throughout the process, created a graphic depiction of the model, and developed an ongoing evaluation process. Each step helped us prepare, initiate, modify, and implement the PPM.
Literature review
A literature review serves as a foundation for the creation of the PPM, ensuring the model is based on strong evidence. We conducted a literature search by identifying key search terms, including publications within the past 5 years, and searching peer-reviewed nursing journals. Because our 5-year cutoff yielded only a few articles that provided insight into the characteristics and essential elements of the PPM, we expanded the literature search to include articles published in the last 10 years.

Key attributes
Key attributes of the PPM should reflect the values, mission, and vision of the organization. We used criteria identified by Hoffart and Woods to develop the key attributes of our PPM. They include professional values, management approach, professional relationships, patient care delivery system, and compensation and rewards. (See Key attributes of a PPM.) We used these same criteria at the evaluation stage.
Nurse engagement
Nurse engagement at every stage of PPM development, implementation, and evaluation ensures buy-in throughout the organization. An example of nurses’ input into our PPM was their request to include the Roy Adaptation Nursing Theory.
We engaged nurses in our PPM process by disseminating surveys through our shared governance structure, which includes Magnet Champions who represent all units, as well as cluster representatives for each major service line, the professional development council, practice council, quality improvement council, advanced practice nurse council, nursing research council, executive council, educators, and unit coordinators.
All council members received information about the PPM with an invitation to actively participate in shaping and modifying it. Face-to-face sessions with Magnet Champions and other interested staff provided the opportunity to brainstorm, discuss, evaluate, and approve all changes.
Multiple references support modifying a PPM as the organization’s landscape, culture, vision, and focus change, so we invited the organization’s to formally evaluate the PPM at various stages of the process.
Graphic depiction
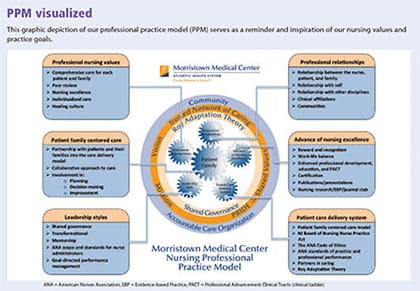
A graphic depiction of the PPM serves as a reminder of nursing values and practice. We collaborated with graphic experts to help create a meaningful illustration of our PPM. Several iterations of the graphic took place before it was finalized. The team voted to add call-out boxes to further explain the components and terms used in the PPM. (See PPM visualized.)
Evaluation
A formal evaluation process allows direct care nurses and nurse managers to review and approve the PPM. Using the criteria we established as our key attributes, we developed a scoring tool for evaluation and revision. The model was complete after repeat surveys and discussion sessions indicated that it accurately reflected the values and culture of the nursing staff throughout the organization.
Key takeaways
To the extent that a PPM guides nurses as they care for patients, families, and community members, it must change as the environment changes, or as the strategy of the organization evolves. Model evaluation should occur at regular intervals, as well as when major changes in care delivery or healthcare landscape occur. Proposed changes can be initiated by direct care staff or leadership, and they should be vetted through a shared governance structure or other mechanism that involves representatives of direct care nurses and members of the interprofessional teams.
In late 2015, our healthcare system, now made up of five hospitals, had a change in senior leadership. At a strategic planning meeting, the phrase Trusted Network of Caring® was coined to reflect our desire to align and focus the system on the care of patients in a manner that instills trust. Although not a major change in our values, we wanted to incorporate the Trusted Network of Caring into the PPM. The inclusion keeps it top of mind, and provides a springboard for proactive transitional care by clinical nurses.
The Trusted Network of Caring framework paves the way for our nursing and interprofessional colleagues to collaborate with other system medical centers to integrate clinical practices, forming a network of resources for the community. Shared services within the community include wound care, a falls committee, and palliative care.
Capturing the culture and focus
Creating, evaluating, and adapting a PPM is an exciting ongoing opportunity for nurse leaders to hear from nurses at all levels. Shaping a PPM motivates staff nurses, allowing them to identify and share priorities that are grounded in the larger organization’s mission and vision.
Changes in strategic direction for systems or organizations necessitate re-evaluating an existing PPM and provides a platform for nurses to incorporate system changes in a meaningful way. Evaluating a PPM in the absence of major strategic changes prompts reinforcement of existing values.
A PPM is a resource for clinical nurses, managers, and professional colleagues specific to their organization. It captures the culture and focus of nurses as it depicts their interactions with patients and coworkers to provide safe, quality care.
Both authors work at Morristown Medical Center in Morristown, New Jersey. Wendy Silverstein is manager of shared governance, nursing education and Magnet, and Mildred Ortu Kowalski is the nurse researcher.
Selected references
American Nurses Credentialing Center (ANCC). ANCC Magnet® Application Manual. MD: ANCC; 2014.
Chamberlain B, Bersick E, Cole D, et al. Practice models: A concept analysis. Nurs Manage. 2013;44(10):16-8.
Harwood L, Downing L, Ridley J. A renal nursing professional practice model: The next generation. CANNT J. 2013;23(3):14-9.
Hoffart N, Woods CQ. Elements of a nursing professional practice model. J Prof Nurs. 1996;12(6):354-64.
McGlynn K, Griffin MQ, Donahue M, Fitzpatrick JJ. Registered nurse job satisfaction and satisfaction with the professional practice model. J Nurs Manag. 2012;20(2):260-5.
Slatyer S, Coventry LL, Twigg D, Davis S. Professional practice models for nursing: A review of the literature and synthesis of key components. J Nurs Manag. 2016;24(2):139-50.
Magnet Stories ANT September Journal


















