Last week I opened the discussion on menopause by addressing demographics. This week I want us to consider what an aging population means in terms of changes in housing requirements, land use, medical care, recreational facilities, rehabilitation centers, retirement, health insurance and costs, senior centers, long-term care facilities, and so forth. On the flip side, a smaller younger population carries an ever-increasing financial burden, and the generation gap becomes a potential burden on all.
No wonder politicians on both sides of the U. S. Congress are arguing about Medicare, Social Security, and health insurance. Not to worry, I do not intend to get into politics at all. But I do have to be a realist, and state categorically that we face a tide of misery unless radical actions are taken in regard to healthcare.
Menopause as a marker in the female life cycle offers one opportunity that public policy experts and politicians should grab – to reduce long-term health costs by enhancing health-related quality of life. But it highlights a very significant Catch-22.
The catch-22 in our fractured US health system is called preventive care. In truth, there is little we can do to truly prevent (if that really means stopping the likelihood of it ever occurring), apart from some of the remarkable vaccines against infections. What we can do for many of the most prevalent of the diseases of older age is reduce the likelihood of getting them, or at least reduce the severity and the complications. But that is not the catch-22.
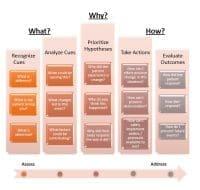
No, this is a much more serious issue. Let me give a very personal experience that explains the dilemma quite dramatically. I was invited some years back to give a lecture in Los Angeles at a dinner meeting that was preceding a major conference for executives of health insurance companies, management care organizations, healthcare facilities, private hospital groups, the pharmaceutical industry, and others. I was seated at dinner with the CEO of one of the nation’s largest providers of health insurance (who shall remain nameless, because his response reflects the nature of the beast we are facing). After the main course, I was invited to speak, which I did on my favorite topic of using menopause as a marker to bring women back into the health care system; most withdraw after they have completed childbearing and do not return unless ill. The purpose from a public health policy perspective is to utilize the menopause as an entry point into a comprehensive screening program to identify risk for future disease or early stages of existing disease. The sooner preventive measures or early treatments are introduced, the greater the likelihood of reducing the serious outcomes, which also happen to be the most expensive procedures for those diseases. In other words, an ounce of prevention could save a pound of treatment.
Quite pleased with myself that I had given one of my better performances, I sat down again at my table. The CEO addressed me immediately. “You know, Wulf, I completely agree with you about the need for population screening and early introduction of appropriate measures. But of course you must realize that all the bad diseases that you are aiming at, like broken hips, heart attacks, Alzheimer’s disease and so on, only truly present themselves in older populations, that is over age 65. That is Medicare. That is the government’s dime. Why should my company spend money up front on prevention when the government will pay for treating the diseases later? It is just not sound business!”
I was floored, and put off eating my dessert. The fact is that barely 1% of our entire healthcare expenditure goes out on preventive care, and that is the truth.
Not surprising then that our health system is so well organized for what I call “crisis care.” Suffer a heart attack on Main Street and an emergency team will be there in minutes, usually getting you rapidly to an Intensive Care Unit, where the best modern care will be available. Hopefully, of course, you have health insurance. But if your clinician prescribes a medication for preventive healthcare, then almost certainly your health insurance will deny payment.
So here is the catch-22 of appropriate menopause management. Menopause is the perfect opportunity to check for risk factors and undiagnosed disease. But the medical insurance industry has little incentive to spend money in the present for complications of diseases that will mostly express themselves after age 65, which is when Medicare covers them. So if you get the tests before 65, the insurance company usually will not pay. If you don’t get an early diagnosis for risk of a disease, or an early stage of established disease, and immediate implementation of appropriate care, the complications and outcome will be worse later. And the treatment will usually be more expensive. The catch-22 is a sick healthcare industry.
Perhaps it is time for the veritable army of menopausal women to get militant and demand of their politicians and policy makers that our healthcare system be brought into the modern age for everyone by including a fair share for preventive care!
DISCUSSION POINTS
1. Do you agree that the increasing proportion of older people in the general population is of importance?
2. How much emphasis is placed on preventive healthcare in the health care system in which you work?
3. Do you think you are doing enough in counseling patients about preventive care?
From next week I will begin to address more specific issues at the individual level: what the menopause really is, the associated early and late health consequences, and the possibilities for enhancing quality of life through appropriate changes in personal behavior and appropriate medical management.
Wulf Utian MD PhD DSc
Author; CHANGE YOUR MENOPAUSE – Why one size does not fit all. https://www.amazon.com/Change-Your-Menopause-size-does/dp/0982845723/