Clinical and community partnerships reduce hospitalization and emergency department visits.
Takeaways:
- Nurses need to lead the way in redesigning integrated healthcare delivery.
- Building relationships and navigating with patients across the care continuum identifies gaps in care coordination.
- Success with value-based payment depends on community-based interprofessional collaboration.
By Billie Lynn Allard, MS, RN
Healthcare delivery in the United States is not sustainable in its present state, and nurses across the country need to take the lead in redesigning it. One group of clinical nurse specialists is spearheading the design and implementation of value-based, integrated care in rural Vermont.
Making the transition
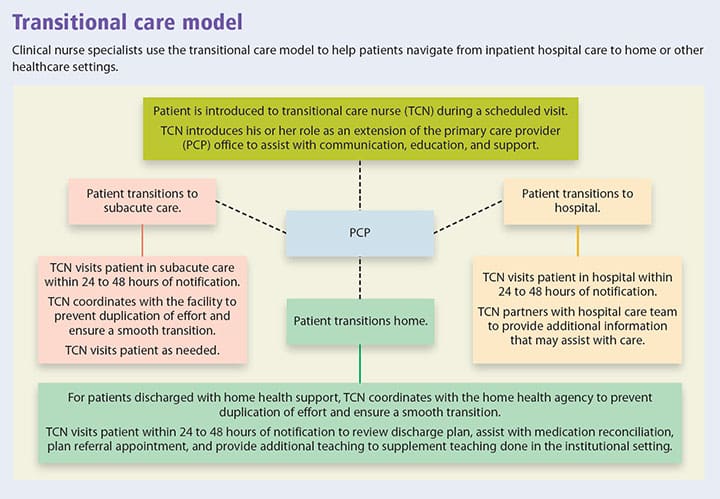
The clinical nurse specialists in our American Nurses Credentialing Center Magnet® designated hospital are integral members of the care team, but with decreasing inpatient census we risked losing this valuable resource. To retain these care professionals, we began a literature search that revealed the successful work of Mary Naylor at the University of Pennsylvania. Naylor used nurse practitioners as transitional care nurses (TCNs) to help patients navigate from one setting to another, bridging the gaps in communication, collaboration, and education. TCNs partner with patients and families, sharing pertinent information with care providers, assisting with appropriate referrals, and providing education about symptom and medication management for chronic diseases. (See Transitional care model.)
Building relationships
With a goal of engaging clinical and community partners in this program, TCNs initially met with the clinical leaders of community agencies and the hospital to identify gaps in care. Then TCNs held group meetings with frontline staff from those facilities and agencies, asking where they saw gaps, where they needed help, and what was and wasn’t working. Getting to know colleagues who play major roles in care delivery and building relationships became the foundation of the project. Home care and medical home agencies worried about duplication of effort and turf issues, so mapping out workflows and providing assistance when requested was the first step. We wanted to create a cohesive, interdisciplinary team to better meet our community’s needs.
Solving the puzzle
 After learning where help was needed, TCNs began spending time in skilled nursing facilities, shadowing home care and hospice nurses, learning about case management, and witnessing care delivery in primary care practices. The total picture of each individual patient’s journey became clearer; TCNs learned that a hospital stay is one small part of the story, with a minimal impact on health outcomes.
After learning where help was needed, TCNs began spending time in skilled nursing facilities, shadowing home care and hospice nurses, learning about case management, and witnessing care delivery in primary care practices. The total picture of each individual patient’s journey became clearer; TCNs learned that a hospital stay is one small part of the story, with a minimal impact on health outcomes.
TCNs discovered that many patients didn’t understand their complex discharge plans, didn’t take medications correctly, and had overwhelming social issues including needing assistance to pay for medications, food, and heat for their homes. The expectation that patients would understand their chronic disease and manage their symptoms was unrealistic. For the first time, the pieces of the puzzle came together.
Measuring results
In the 3 years since this project began, all primary care practices affiliated with the Southwestern Vermont Health Care system have chosen to partner with the TCNs. Each TCN works with three to four primary care practices, identifying high-risk, chronic care patients who’ve had multiple hospitalizations and emergency department (ED) visits and may benefit from assistance. More than 1,000 patients have participated in the program with over 700 allowing home visits.
Implementing TCNs led to a 49.7% decrease in hospitalizations and a 11.3% decrease in ED visits in the 180 days after intervention among these patients. Scores on satisfaction surveys are high, with multiple positive comments from patients and families, and healthcare costs for patients in the program have fallen. Reduced rates of hospitalization and ED visits mean less revenue for the hospital, a goal for healthcare reform that’s difficult to embrace in a fee-for-service model, but will be rewarded in a value-based environment.
As part of annual nursing education, the TCNs have shared insights with their inpatient colleagues. As a result, projects are underway to change how we discharge patients and involve them in the process:
- creating refrigerator magnets with color-coded instructions for managing chronic obstructive pulmonary disease (COPD) and heart failure symptoms in all settings
- providing medication boxes along with assistance from healthcare providers to educate patients about proper use
- partnering with clinical pharmacists to ensure cost-effective medication ordering and to develop strategies that improve medication adherence, such as pharmacists providing medication education in hospitals, primary care practices, and homes
- sharing standardized heart failure, COPD, and diabetes education with providers in various healthcare settings to improve patient understanding.
The team creates care plans that better meet the needs of their patient population; interventions include helping patients find stable housing situations, procure health insurance, establish primary care providers, and find part-time jobs. Diabetes educators are embedded in office practices to engage patients in shared goal setting, to teach disease-management skills, and to support patients with new and existing diagnoses. Patients enrolled in the integrated diabetes education program had a 15.7% reduction in their average HbA1c levels.
At weekly transitional care team meetings and quarterly community-based meetings, the team gathers information, updates the gap analysis, and systematically creates an accountable community of care. (See A community of care.)
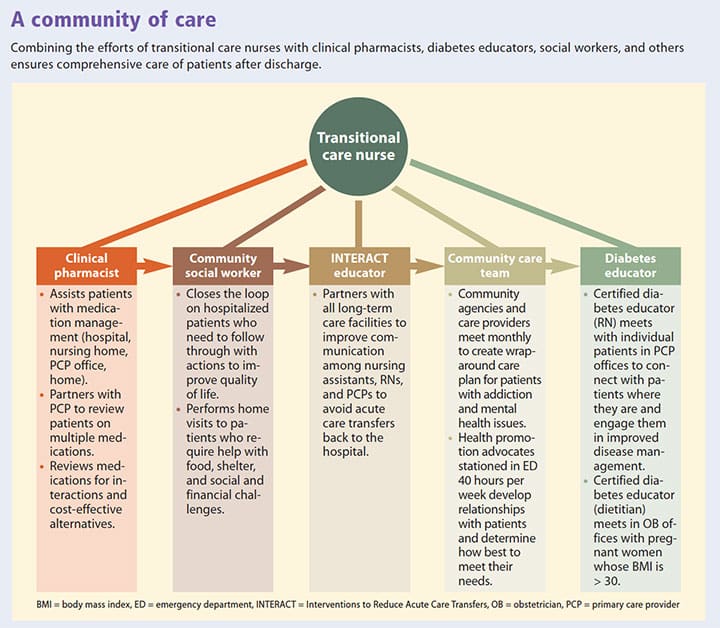
Strengthening partnerships
The TCNs’ work has strengthened partnerships with ambulatory practices by reducing gaps in care coordination. Primary care providers also have more resources at their fingertips. For example, a provider can reach out to a TCN and request a home visit for a woman whose blood glucose and blood pressure are out of control but who claims to be taking her medications. During the home visit, the TCN may discover the patient never filled the prescription for a diabetes medication and is taking only half of the blood pressure medication because of the side effects. The TCN then communicates that information to the medical home nurse case manager, who shares it with the provider.
TCNs visit patients 24 to 48 hours after discharge to review instructions and medications and to ensure a safe home environment. The TCN shares updated information with the primary care provider before the patient’s next office visit along with questions and concerns to be addressed during the appointment. TCNs may accompany patients to provider appointments, sharing crucial information, updating medication lists, and ensuring patients understand instructions and medication changes. For example, the TCN might supervise a man with heart failure correctly adding new cardiac medications and removing others from his medication box, explain what the new medication is for, and discuss the importance of daily weights. The TCN leaves his or her contact information in case the patient has any questions or concerns and then returns in 3 days for a follow-up visit. The goal is to help patients own their health and better understand how their decisions and choices have consequences. Some patients require only one or two home visits, while others benefit from 3 or 4 months of oversight.
The transitional care program offers nurses the opportunity to partner over time with individual patients and their families to develop trusting relationships. We strive to meet patients where they are, find out what their goals are for the future, and help them develop a realistic plan to get there. When necessary, TCNs assist with palliative care or hospice referrals, laying the foundation for the next choice the patient makes. Care is driven by the patient and supported by the nurse.
Making an impact
TCNs are making an impact on the delivery of healthcare in this community and meeting the triple aim (improving the patient experience, improving population health, and reducing per capita healthcare costs). Patient surveys demonstrate improvement in the patient experience, quality outcomes have improved, and hospitalizations and ED visits have steadily decreased for patients in the program. Even more important is the interdisciplinary team approach to care delivery. We’re using available, appropriate resources, creating a shared care plan, and advocating as one for necessary resources. One by one, we’re bridging gaps to improve healthcare delivery in our community. Without a doubt, it’s the most meaningful and rewarding work of our careers.
Billie Lynn Allard is the administrative director of care management, transitional care, and ambulatory services at Southwestern Vermont Health Care in Bennington.
In October 2017, Southwestern Vermont Medical Center received $50,000 for this innovation as the winner of the ANCC Magnet Prize™, sponsored by Cerner.
Selected references
American Nurses Association. The value of nursing care coordination. 2012.
Brock J, Mitchell J, Irby K, et al; Care Transitions Project Team. Association between quality improvement for care transitions in communities and rehospitalizations among Medicare beneficiaries. JAMA. 2013;309(4):381-91.
Cipriano P. The imperative for patient-, family-, and population-centered interprofessional approaches to care coordination and transitional care: A policy brief by the American Academy of Nursing’s career coordination task force. Nurs Outlook. 2012;60(5):330-3.
Clarke R, Bharmal N, Di Capua P, et al. Innovative approach to patient-centered care coordination in primary care practices. Am J Manag Care. 2015;21(9):623-30.
Dreyer T. Care transitions: Best practices and evidence-based programs. Home Healthc Nurse. 2014;32(5):309-16.
Farrell TW, Tomoaia-Cotisel A, Scammon DL, et al. Impact of an integrated transition management program in primary care on hospital readmissions. J Healthc Qual. 2015;37(1):81-92.
Goodman DC, Fisher ES, Chang CH. The Revolving Door: A Report on U.S. Hospital Readmissions. Robert Wood Johnson Foundation/The Dartmouth Institute; 2013.
Hacker K, Walker DK. Achieving population health in accountable care organization. Am J Public Health. 2013;103(7):1163-7.
Labson MC. Adapting The Joint Commission’s seven foundations of safe and effective transitions of care to home. Home Healthc Now. 2015;33(3):142-6.
Labson MC. Innovative and successful approaches to improving care transitions from hospital to home. Home HealthC Now. 2015;33(2):88-95.
Naylor MD, Bowles KH, McCauley KM, et al. High-value transitional care: Translation of research into practice. J Eval Clin Pract. 2013;19(5):727-33.
ant1-Magnet Stories-1221


















