With accurate diagnosis, patients can be appropriately treated in and out of the hospital.
Takeaways:
- The estimated cost of treating community-acquired pneumonia (CAP) in the United States is $12.2 billion a year
- Risk factors for CAP include antibiotic treatment, chronic steroid use, and malnutrition.
- Diagnostic tools aid in determining whether CAP treatment can be provided in the outpatient setting or if hospitalization is required.
By Shari J. Lynn, MSN, RN
Community-acquired Pneumonia (CAP) is exactly what it sounds like—a lung infection acquired while out and about in the world. The cause may be a virus, bacteria, or fungus. (See CAP stats.) 
The estimated cost of treating CAP in the United States is about $12.2 billion a year. Inpatient treatment ranges from $7,500 to $10,227 per admission, whereas outpatient treatment ranges from $150 to $350 per patient. This difference demonstrates the need for accurate diagnosis and appropriate treatment.
Immune response
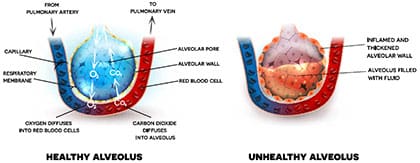
A patient’s immune response to CAP depends on the type of organism involved. Less noxious organisms typically are destroyed by macrophage engulfment, which results in a moderate immune response. If the organism is highly virulent or is present in great numbers, a series of immune responses occur, including inflammation, cellular infiltration, and activation of the immune cascade. When the patient can’t clear pulmonary secretions, a secondary infection may develop. (See Immune response.)
 In response to physiologic changes, the patient’s respiratory rate may increase in an attempt to improve oxygen levels, but eventually he or she becomes exhausted from the work of tachypnea, and the respiratory rate decreases, leading to hypoxemia and hypercapnia. In addition, the patient may experience fever, pleuritic chest pain, coughing, dyspnea, and a general feeling of being unwell. In older adults, symptoms may not be as obvious; they may have a less productive cough, anorexia, or confusion.
In response to physiologic changes, the patient’s respiratory rate may increase in an attempt to improve oxygen levels, but eventually he or she becomes exhausted from the work of tachypnea, and the respiratory rate decreases, leading to hypoxemia and hypercapnia. In addition, the patient may experience fever, pleuritic chest pain, coughing, dyspnea, and a general feeling of being unwell. In older adults, symptoms may not be as obvious; they may have a less productive cough, anorexia, or confusion.
Risk factors
Many factors contribute to an increased chance of developing CAP. (See CAP risk factors.) Antibiotic treatment, chronic steroid use, and malnutrition increase the risk for CAP, as do comorbidities such as chronic renal failure. In the elderly population, comorbidities as well as the effects of aging (such as reduced mucociliary movement and clearance, decreased cough reflex, increased potential for colonization of gram-negative organisms, and decreased immune response) increase the risk for CAP. Additional risk factors include spleen removal, HIV, hypogammaglobulinemia, and sickle cell disease.
Classification and causes
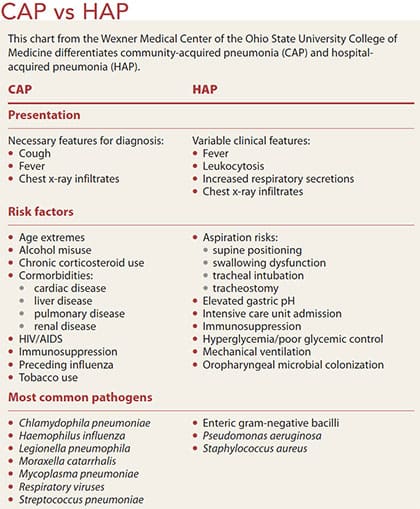
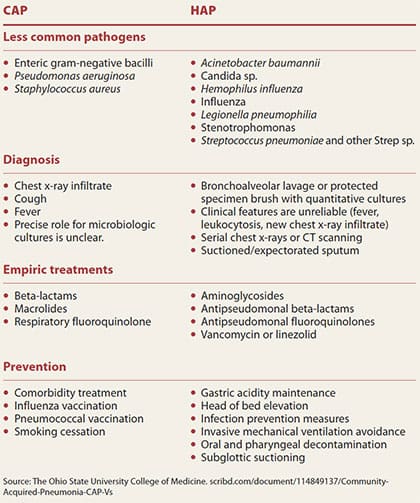
CAP is just one classification of pneumonia. (See CAP vs. HAP.)
The criteria for CAP include:
- patient hasn’t been hospitalized within 14 days before symptom onset
- patient’s symptoms begin within 4 days of hospital admission
- patient doesn’t live in a longterm care facility.
Bacterial pathogens and respiratory viruses are common causes of CAP. Bacterial organisms that are treatable in the outpatient setting include Chlamydophila pneumoniae, Haemophilus influenzae, Moraxella catarrhalis, Mycoplasma pneumoniae, and Streptococcus pneumoniae. Respiratory viruses associated with outpatient treatment of CAP include adenovirus, influenza A and B, parainfluenza virus, and respiratory syncytial virus. However, any patient infected with these pathogens who shows severe symptoms may be admitted for inpatient care as well as those infected with anaerobes that are related to aspiration and Legionella pneumophila.
Patient assessment
Begin the patient assessment by identifying symptoms and their onset. Note symptom severity, including characteristics of cough and sputum, descriptions of pain level, factors that relieve or aggravate symptoms, treatments the patient has already tried, and how the patient describes illness severity.
Negative test results and negative symptoms can help rule out other diagnoses. Ask about abdominal pain, chest pain, hematuria, dysuria, edema, weight gain, and neurological symptoms. In addition, gather information about the patient’s current medications (including prescription and over-the-counter medications and herbal remedies); tobacco, alcohol, and illicit drug use; environmental exposure to possible lung irritants; and immunizations.
Note allergies and past medical history as well as social and family histories. Ask about any comorbidities, such as cancer, autoimmune disease, and chronic respiratory issues. Also note the patient’s residence (for example, home or longterm care facility).
Examine all body systems to determine infection severity, the probability of CAP, and other illnesses that may have contributed to CAP. A head, ears, eyes, nose, and throat exam may reveal an upper- respiratory infection related to nasal congestion, ocular discharge, mouth breathing, nasal flaring, or otitis media. Dullness and dryness of the lips, eyes, and mucosa may be signs of dehydration.
Pulmonary auscultation and physical examination may reveal dull percussion, chest tenderness, increased tactile fremitus, bronchoph ony, egophony, and whispered pectoriloquy. You also may hear wheezes, rhonchi, or crackles, and the patient may have pleuritic chest pain that’s more severe on deep inspiration.
Cardiovascular effects of CAP include poor perfusion, prolonged capillary refill, and tachycardia. Because of dehydration and cyanosis caused by hypoxia, the patient’s skin may tent, and he or she may experience men tal status changes. Changes in mental status, loss of appetite, and falls (related to confusion and dizziness as a result of hypoxia) also can be factors that are part of a CAP diagnosis.
Diagnostic tools
Diagnosis of CAP includes a chest x-ray. Viral pneumonia commonly presents with interstitial infiltrates on x-ray; bacterial infection presents with alveolar infiltrates. Viral and bacterial infections can occur simultaneously.
Many tools (including the pneumonia severity index, CURB-65 and CRB-65, SMART COP, and the American Thoracic Society criteria) are available to help determine if the patient with CAP can be treated successfully as an outpatient or if hospital admission is required.
Pneumonia severity index
The pneumonia severity index (PSI) was developed to classify patients suspected of having CAP. This tool, which has been used in emergency departments, nursing homes, and community hospitals, looks at patient characteristics such as:
- demographics (gender and residence)
- physical assessment findings (mental status, pulse, respiratory rate, temperature, and systolic blood pressure)
- laboratory results (pH, blood urea nitrogen [BUN], sodium glucose, hematocrit, and partial pressure of arterial oxygen)
- comorbidities (liver disease, neoplasm, stroke, heart disease, and renal failure)
- radiology results (presence of pleural effusion).
PSI scoring places patients into one of five categories. The first three recommend outpatient treatment; the fourth and fifth recommend hospitalization.
CURB-65 and CRB-65
CURB-65 and CRB-65 are easier to use than the PSI. Although the PSI has 20 items, CURB-65 has only five (confusion, BUN > 19 mg/dL, respiratory rate > 30 breaths/ minute, systolic blood pressure < 90 mmHg or diastolic blood pressure < 60 mmHg, and age > 65 years) and CRB-65 has only four (the same items as CURB 65, but BUN isn’t necessary if lab results aren’t available). To view the CURB-65 and CRB-65 tools.
Both tools result in a rating that corresponds to patient care recommendations. CURB-65 rates patients with 0 or 1 as being acceptable for outpatient treatment; 2 as short inpatient stay or closely supervised outpatient treatment; and 3, 4, and 5 as hospitalization and possible ICU admission. CRB-65 rates patients as 0 (no need for hospitalization), 1 to 2 (consider hospitalization), and 3 to 4 (urgent recommendation for hospitalization).
SMART-COP
SMART-COP is used to determine the severity of CAP in adults. The acronym represents the information needed to make the proper determination for care, and the data collected translates to a point system. Scoring for a patient who is under 50 years old is:
Systolic blood pressure < 90 mmHg (2 points)
Multilobar chest x-ray involvement (1 point)
Albumin < 35 g/L (1 point)
Respiratory rate ≥ 25 breaths/minute (1 point)
Tachycardia ≥ 125 beats/minute (1 point)
Confusion—acute (1 point)
Oxygen—low arterial oxygen pressure (PaO2) ≤ 70 mmHg or oxygen saturation ≤ 93% or PaO2/fraction of inspired oxygen (FiO2) < 333 mmHg (2 points)
pH < 7.35 (2 points).
For patients over 50, all the factors are the same except respiratory rate (> 30 breaths/minute) and oxygen level (PaO2 < 60 mmHg or oxygen saturation ≤ 90% or PaO2/FiO2 < 250 mmHg).
The total score determines the patient’s risk for needing intensive respiratory vasopressor support.
0-2 = low risk
3-4 = moderate risk
5-6 = high risk
7 = very high risk
Patients with a score of ≥ 5 are considered to have an increase risk for CAP.
American Thoracic Society criteria
The American Thoracic Society has created criteria for patients with severe CAP who require ICU admission.
Minor criteria include:
- respiratory rate > 30 breaths/minute and PaO2/FiO2 ≤ 250 mmHg (A need for noninvasive ventilation can substitute for a respiratory rate > 30 breaths/minute or PaO2/FiO2 mmHg < 250.)
- multilobar infiltrates
- confusion/disorientation
- uremia (BUN level ≥ 20 mg/dL)
- leukopenia as a result of the infection alone (white blood cell count < 4,000 cells/mm3)
- thrombocytopenia (platelet count < 100,000 cells/mm3)
- hypothermia (core temperature < 96.8° F [36° C])
- hypotension requiring aggressive fluid resuscitation.
Major criteria include:
- invasive mechanical ventilation
- septic shock with the need for vasopressors.
Other criteria to consider include hypoglycemia (in patients without diabetes), acute alcoholism or alcohol withdrawal, hyponatremia, unexplained metabolic acidosis or elevated lactate level, cirrhosis, and asplenia.
Nursing interventions and treatment
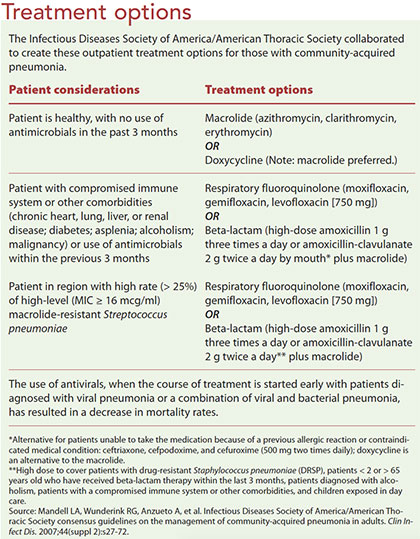
In the outpatient setting, patients with CAP are treated with antibiotics as outlined in guidelines from the American Thoracic Society and the Infectious Diseases Society of America. (See Treatment options.) With the increase in antibiotic resistance, evidence-based prescribing is crucial. To decrease the chance of antibiotic-resistant microorganisms developing and to reduce the chances of adverse effects from antibiotic treatment, a short (5-day) course of antibiotic treatment is recommended. Research shows no difference between long- and short -course antibiotic treatment of CAP, and the short course has been shown to reduce the risk of Clostri diumdifficile.
To qualify for short-course antibiotic treatment, patients must be deemed clinically stable by the health care provider. The definition of clinically stable includes 48 to 72 hours without a fever in the last 5 days of therapy, systolic blood pressure > 90 mmHg, heart rate < 100 beats/minute, respiratory rate < 24 breaths/minute, oxygen saturation > 90%, and normal mental status. If no improvement occurs after 5 days of antibiotic use, treatment should continue for another 2 days.
Recent research provides a better understanding of CAP patients receiving current treatments as compared to health care-associated pneumonia patients, specifically related to CAP drug-resistant pathogens (CAP-DRP), including Pseudomonas aeruginosa, Acinetobacter baumannii, methicillin-resistant Staphylococcus aureus (MRSA), and extremely resistant Enterobacteriaceae.
The goal of this research is to decrease the overuse of narrowspectrum antibiotics, which can result in using inappropriate medications and broad-spectrum antibiotics. (See Drug-resistent pathogen algorithm.)
Other treatments include acetaminophen for pain and fever, early ambulation, appropriate hydration, and nutritional meals. Systemic steroids (if reactive airway involvement secondary to CAP exists), bronchodilators, and cough suppressants may also be ordered.
Teach patients the expected guidelines for recovery, which include:
- fever resolved in 1 week
- notably decreased chest pain and sputum in 4 weeks
- notably decreased cough and breathlessness in 6 weeks
- resolution of symptoms (although fatigue may still be present) in 3 months
- feeling back to normal in 6 months.
Patients with underlying comorbidities may follow a different or extended course of recovery.
Follow-up for outpatient treatment is usually 48 to 72 hours after the initial diagnosis, with another follow-up appointment with the healthcare provider in 2 to 3 weeks. Instruct patients to contact their provider if any unexpected complications develop. Patients who smoke should have additional follow- up at the 6- to 12-week mark for a repeat assessment and chest x-ray to rule out underlying pathology that may have been a factor in the original CAP diagnosis.
What’s in your toolkit?
Using tools to assess whether CAP patients can be treated in the community reduces care costs and protects patients with decreased immunity from being ad mitted to hospitals, where they may acquire other infections. The assessment tools lead to treatment designed to limit the creation of additional drug-resistant patho gens. Research regarding CAP is fluid, so stay up-to-date with the most recent evidence-based practices.
Shari J. Lynn is an instructor at the Johns Hopkins University School of Nursing in Baltimore, Maryland.
Selected references
Almatar MA, Peterson GM, Thompson A, McKenzie DS, Anderson TL. Community-acquired pneumonia: Why aren’t national antibiotic guidelines followed? Int J Clin Pract. 2015;69(2):259-66.
Arshad H, Fasanya A, Cheema T, Singh AC. Acute pneumonia. Crit Care Nurs Q. 2016;39(2):148-60.
Driver C. Pneumonia part 1: Pathology, presentation and prevention. Br J Nurs. 2012;21(2):103-6.
Gibson V. Recognising and managing community-acquired pneumonia. Nurs Stand. 2015;30(12):53-9.
Mandell LA, Wunderink RG, Anzueto A, et al. Infectious Diseases Society of America/American Thoracic Society consensus guidelines on the management of community-acquired pneumonia in adults. Clin Infect Dis. 2007;44(suppl 2):s27-72.
Severson C, Renstrom C, Fitzhugh M. Health promotion, risk stratification, and treatment options to decrease hospitalization rates for community-acquired pneumonia in adults. J Am Assoc Nurse Pract. 2014;26(10):537-49.
Therapeutic Guidelines. SMART-COP tool for assessing severity of community-acquired pneumonia (CAP) in adults. 2010.
Wunderink RG. Community-acquired pneumonia versus healthcare-associated pneumonia. The returning pendulum. Am J Respir Crit Care Med. 2013;188(8):896-8.



















3 Comments.
As noted above.
This education articles provided a lot of great information!!
As I am reading this article, the news here in New Orleans, Louisiana states, ” Louisiana is leading the nation in the FLU” . I am presently on the tail end of a simple cold.
Thank you for your Mindfulness as it relates to CAP, and nursing interventions to help my community prevent rebound effects of improper use of Antibiotic Therapy as we together fight CAF ( Community – Acquired FLU. )