Older adults make up 13% of the U.S. population but account for 36% to 50% of hospital admissions and 44% of hospital charges. About 20% of Medicare patients are readmitted within 30 days; an estimated 75% of these readmissions are preventable.
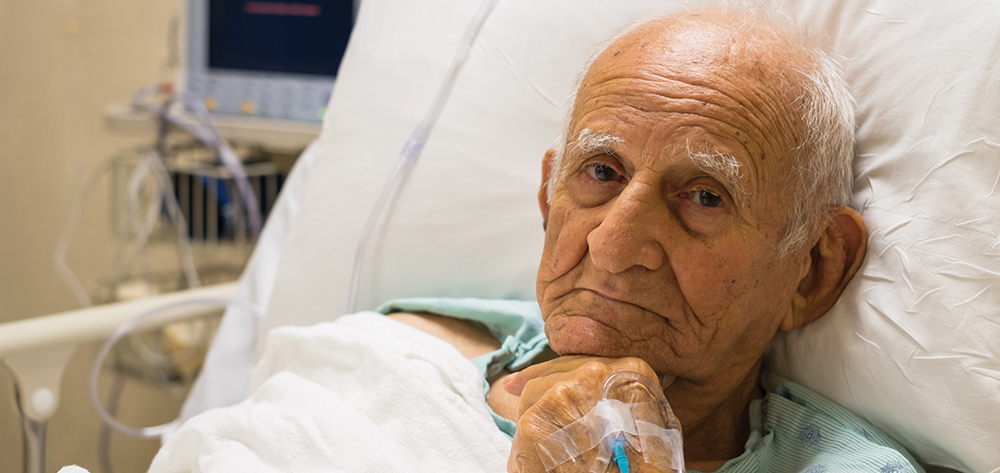
A dramatic event at any age, hospitalization poses unique challenges for older adults. Hospitals harbor such dangers as adverse drug events, restraint injuries, and falls, which can be lethal in the elderly. For these patients, hospitalization also is linked to a significant risk for delirium, malnutrition, infection, and loss of functional independence—possibly leading to persistent disability, nursing home placement, and death. Evidence-based nursing care models to prevent these complications continue to gain support. Many of these models embrace multidisciplinary assessment, communication, and coordination.
Hospitalized older adults have an uncertain trajectory; many never regain their previous mobility. Some studies show up to 35% of older hospitalized patients experience a decline in baseline activities of daily living (ADL) after admission.
As a nurse, you can help prevent patients from leaving the hospital with worse function than they came in with. You’re in a pivotal position to observe their independence level in performing basic ADLs. A standardized screening instrument, such as the Katz Index of Independence in Activities of Daily Living (bathing, dressing, toileting, eating, and transfer), can help the healthcare team identify deficits and plan posthospital care. Mobility routines that include getting the patient up for meals or sitting in a recliner or rocking chair may improve mobility among weak or fatigued older adults.
This article discusses some of the hidden dangers of hospitalization for older adults—delirium, reduced mobility and falls, malnutrition, dehydration, and infections.
Delirium
The hallmark of certain acute illnesses, delirium or acute confusion is the leading complication of hospitalization in older adults. It affects 25% to 60% of older hospitalized adults in the United States and costs about $8 billion yearly.
The complex pathophysiology of delirium includes neurotransmitter alterations. Processes that may contribute to delirium include hypoxia, infection, electrolyte imbalance, constipation, and pain.
The good news: Delirium may be preventable in at least 40% of cases. Assess all hospitalized older adults for confusion during each shift, noting inattention or fluctuating mental status. Ask them what brought them to the hospital and ask them to name the days of the week or months of the year forward and backward. If you note changes, document these and discuss them with all care team members.
Try to identify the cause of delirium. Know that restraints and certain medications can prolong or worsen this condition. If you note sudden or worsening confusion in a patient with known cognitive impairment, evaluate for potential acute reversible causes.
The following interventions can help prevent delirium in older adults:
- Use appropriate pain medications in dosages tailored to older adults.
- Avoid sleeping medications.
- Correct sensory deficits, such as hearing and vision loss.
- Encourage increased visits from family members and volunteers.
- Provide access to music and art therapy.
- Create a quiet environment for sleep at night.
An “aging tool kit” that includes hearing amplifiers and magnifying glasses can be assembled to enhance communication and provide safe options for distraction, including books and puzzles.
Reduced mobility and falls
The hazards of immobility and prolonged bed rest have been known for decades. Many healthcare professionals have noted the negative effects of bed rest, including orthostatic hypotension, atelectasis, decreased muscle strength, increased bone loss, constipation, incontinence, pressure ulcers, and confusion.
Maintaining the patient’s mobility is the best way to prevent falls. Provide opportunities to enhance mobility safely. Consult a physical therapist, who can assess for balance and gait abnormalities and provide exercises and equipment to help the patient regain strength, avoid complications, and promote return to baseline function. Use devices such as slings and lifts as needed to move patients so you protect them (and yourself) from injury while still providing opportunities for mobility.
Ensure that the patient has assisted or supervised ambulation (especially to the bathroom). Provide ongoing education to the patient and family, using the teach-back technique, to identity the patient’s safe level of function and encourage exercise and use of mobility aides. For example, tell the patient, “Show me what you would do if you had to go the bathroom.” Or ask, “What would you do if you called for the nurse and she didn’t come immediately?” Suggest that plan B might be to call for the nurse again.
Another way to help prevent falls is proactive rounding to provide assistance for toileting and ensuring a safe environment. Such rounds strongly encourage and assist older adults to go to the bathroom before they feel the urge and need to rush. Other effective interventions include:
- placing frail patients in rooms near the nurse’s station
- keeping the bed in the low position
- keeping the call light, water, and accessories within reach
- using dim lighting at night
- placing furniture in nonobtrusive positions
- raising the toilet seat.
Malnutrition and dehydration
At least half of older adults are admitted to the hospital with dehydration and malnutrition. Both conditions are independent risk factors for falls, confusion, pressure ulcers, impaired immunity, longer stays, and even death.
Assess your patient’s nutritional status on admission to identify and correct nutritional deficits in a timely manner. For lethargic older adults, assess safe swallowing ability at the bedside. During an acute illness, avoid aggressive restricted diets (including nothing-by-mouth) for prolonged periods.
Preventing constipation is crucial. Prevention strategies include providing adequate fluids and warm prune juice and promoting mobility. In some older adults, nutrition can become critical, signaling depression and end-of-life issues. Feeding-tube placement must be evaluated carefully.
Provide nutritional and speech resources to help manage nutritional problems. As needed, arrange for an ethics consultation to give the patient and family the information they need to set realistic goals. Be sure to honor the patient’s wishes.
Other interventions to prevent malnutrition and dehydration include:
- assessing and honoring the patient food’s preferences
- providing a “liberal kitchen” with snacks available 24/7
- performing oral care before meals to help the patient maintain nutrition and prevent infections.
- getting the patient out of bed for meals and for 20 minutes afterward, if possible, to prevent indigestion.
Infections
Older adults with decreased immune function are at special risk for infection. Urinary tract infections and pneumonia commonly necessitate hospital admission in older adults. However, antibiotic therapy to treat infection can be particularly complex in older adults who may have unique illness presentations, are at increased risk for resistant organisms, or are receiving multiple medications that may increase adverse effects.
Also, know that certain hospital routines may pose undue risk of infection. To help decrease the risk of atelectasis and pneumonia, avoid bed rest when possible. Carefully evaluate the need for indwelling urinary catheters, considering their risks, benefits, and alternatives. Discontinue these catheters as soon as possible.
Consider the following interventions as well:
- Remind older adults to perform ongoing oral care, including teeth or denture brushing, mouth rinsing, and lip care for dryness. As needed, assist them with this care.
- Be sure staff and visitors wash their hands before and after contact with the patient.
- Instruct older adults to perform daily hygiene, including hand washing.
The value of discharge planning
Appropriate discharge planning helps avoid functional decline in older adults. Planning for the patient’s discharge begins at the time of admission and must be integrated into daily care by all care providers. Due to insurance requirements and financial constraints, discharge planning has become increasingly complex.
Choices for posthospital care depend on the patient’s health status and illness trajectory, as well as available support persons and resources. The interdisciplinary team must be able to give the patient and family a realistic trajectory of recovery as well as recommended options.
Nurses in all care settings, particularly acute-care hospitals, are well placed to help older adults avoid functional decline. In some cases, this may require a change in the hospital culture and additional education for nurses regarding older adults’ unique needs. Special areas of focus include the patient’s particular needs, care transitions, and possible changes in hospital routines, such as bed rest and restraint use.
Selected references
Agency for Healthcare Research and Quality. National Guideline Clearinghouse. www.
guideline.gov/search/search.aspx?term=older+adults
American Academy of Nursing’s Expert Panel on Acute and Critical Care. Reducing Functional Decline in Older Adults During Hospitalization: A Best Practice Approach. Try This®: Best Practice in Nursing Care to Older Adults General Assessment Series; Issue 31, 2012. Hartford Institute for Geriatric Nursing. www.consultgerirn.org/uploads/File/
trythis/try_this_31.pdf
Asher R. The dangers of going to bed. Br Med J. 1947 Dec 13;2(4536):967-8.
Inouye SK, Bogardus ST, Charpentier PA, et al. A multicomponent intervention to prevent delirium in hospitalized older adults. N Engl J Med. 1999;340(9):669-76.
Landefeld CS, Palmer RM, Kresevic DM, Fortinsky RH, Kowal J. A randomized trial of care in a hospital medical unit especially designed to improve the functional outcomes of acutely ill older patients. N Engl Med. 1995; 332(20):1338-44.
The NICHE Program. Nurses Improving Care for Healthsystem Elders (NICHE). 2015. www.nicheprogram.org/program_overview
Denise M. Kresevic is a geriatric clinical nurse specialist III at University Hospitals Case Medical Center in Cleveland, Ohio, and a geriatric nurse practitioner and nurse researcher at the Louis Stokes Cleveland VA Medical Center.